Abstract
Introduction
For most cancer types, cancer incidence as well as cancer-specific mortality is higher in men compared to women. The underlying reasons for this remain unclear but hypotheses include sex differences in environmental exposure to carcinogens, health-seeking behavior and biology, such as hormonal, anatomical, and molecular disparities. For lymphomas, the impact of sex seems to differ by subtype, treatment, and calendar time. For example, in Hodgkin lymphoma (HL), male sex has historically been considered an established negative prognostic factor but in contemporary studies, therapeutic advances appear to have attenuated the prognostic value of sex. In contrast, a negative impact of male sex on prognosis has become manifest during the last decades in patients with diffuse large B-cell lymphoma and follicular lymphoma, with sex differences in rituximab clearance in elderly proposed as one explanation. Previous studies have not considered the longer life expectancy of women when predicting incidence and prognosis, and comprehensive studies on the impact of sex on incidence and excess mortality in lymphomas are lacking. Therefore, we aimed to quantify and outline sex differences in lymphoma incidence and lymphoma excess mortality by subtype in a large, population-based cohort.
Methods
Adult patients diagnosed with lymphoma 2000-2019 were identified via the Swedish lymphoma register (>95% national coverage). Sex-specific incidence rates were computed as the number of new cancer cases per 100,000 person-years/year and age-standardized to the Swedish population in 2019 (using population counts from Statistics Sweden). Male-to-female incidence rate ratios (IRRs) with 95% confidence intervals (CIs), adjusted for age and year of diagnosis, were estimated using Poisson regression models. Sex-specific 5-year relative survival was calculated as the ratio of the observed lymphoma patient and the matched (sex, age, and calendar year) population 5-year survival and age-standardized according to the International Cancer Survival Standards. Male-to-female 5-year excess mortality rate ratios (EMRR) including 95% CIs were estimated including age and calendar year in the Poisson regression models.
Results
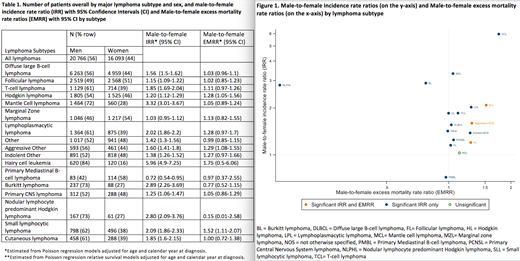
A total of 36 859 patients with lymphoma were identified during the study period. Median age for all patients was 69 (range 16-99) years. In the whole cohort there was a male predominance of 56%. Distribution of patients by sex, and male-to-female IRR and EMRR adjusted for age and year of diagnosis by major lymphoma subtype are presented in Table 1, and graphically in Figure 1. Overall, significantly higher incidence rates among men were observed for all lymphoma subtypes except marginal zone lymphoma and primary mediastinal B-cell lymphoma. The higher male-to-female IRRs remained largely stable over calendar time. For some subtypes, male-to-female IRR differed by age. For example, in HL, male and female IRs were similar up to 35 years, whereafter the male-to-female IRR increased. For both Burkitt lymphoma and Nodular lymphocyte predominant Hodgkin lymphoma the higher male-to-female IRR was most pronounced among patients under the age of 50, although incidence was higher among men of all ages for both subtypes. Regarding survival, there was a trend for higher excess mortality among men for several subtypes (Table 1, Fig 1). Significantly higher EMRRs among male patients were seen in HL, aggressive lymphomas not otherwise specified, and small lymphocytic lymphoma.
Conclusion
In this large population-based study we observe a significantly higher incidence rate among men for all but two lymphoma subtypes. Further, there was a trend for worse survival among male lymphoma patients for most lymphomas although only significantly worse for three subtypes, potentially due to small numbers for rare subtypes and limited adjustment. As of yet, reasons for sex differences in incidence and excess mortality of lymphoma are unknown. Better understanding of underlying factors to these differences may improve management of lymphomas and increase knowledge of lymphoma biology and etiology. Thus, further studies on sex differences in lymphoma with detailed data regarding disease-specific patient characteristics, treatment and patient-related factors such as comorbidity and socioeconomic status are warranted.
Weibull: Jansen-Cilag: Other: part of a research collaboration between Karolinska Institutet and Janssen Pharmaceutica NV for which Karolinska Institutet has received grant support. El-Galaly: Abbvie: Other: Speakers fee; ROCHE Ltd: Ended employment in the past 24 months. Smedby: Jansen-Cilag: Other: part of a research collaboration between Karolinska Institutet and Janssen Pharmaceutica NV for which Karolinska Institutet has received grant support.

This feature is available to Subscribers Only
Sign In or Create an Account Close Modal